ORIGINAL RESEARCH | https://doi.org/10.5005/jp-journals-10077-3081 |
A Comparative Evaluation of CPP-ACP Cream and Fluoride Varnish in Remineralization of MIH-affected Teeth Using Laser Fluorescence
1–4Unit of Pedodontics and Preventive Dentistry, Oral Health Sciences Center, Postgraduate Institute of Medical Education and Research, Chandigarh, India
Corresponding Author: Sanjeev K Singh, Unit of Pedodontics and Preventive Dentistry, Oral Health Sciences Center, Postgraduate Institute of Medical Education and Research, Chandigarh, India, Phone: +91 9780554348, e-mail: san.bajaj88@gmail.com
How to cite this article Singh SK, Goyal A, Gauba K, et al. A Comparative Evaluation of CPP-ACP Cream and Fluoride Varnish in Remineralization of MIH-affected Teeth Using Laser Fluorescence. J South Asian Assoc Pediatr Dent 2021;4(2):117–121.
Source of support: Nil
Conflict of interest: None
ABSTRACT
Background: Molar incisor hypomineralization (MIH) affected teeth have enamel with altered mineral content like decreased calcium, phosphorous, and increased carbon leading to porous enamel and subsequent post-eruptive breakdown. The treatment is aimed at the prevention of their breakdown. Various remineralization strategies originally employed for initial carious lesions have been extrapolated for use on these defects.
Aim and objective: To evaluate the remineralization potential of CPP-ACP-based cream and fluoride varnish for MIH-affected teeth using laser fluorescence (LF).
Materials and methods: Thirty children aged 8–14 years who exhibited intact, demarcated opacities on their first permanent molars or permanent incisors, were randomly divided into two groups using simple randomization technique; group I: professional application of fluoride varnish (n = 15); group II: daily single application of CPP-ACP cream (n = 15). The mineral density was assessed before and after 15 days of application with a DIAGNOdent™ pen (KaVo).
Results: The mean change in LF values depicting a change in the mineral density scores was 8.933 ± 5.05 for the fluoride varnish group and 7.133 ± 4.17 for the CPP-ACP group. This decrease was statistically significant for both groups. However, no significant difference was found between the two groups in terms of these changes.
Conclusion: Both CPP-ACP cream and fluoride varnish are equally effective in achieving remineralization of MIH-affected teeth.
Keywords: CPP-ACP, Fluoride varnish, Laser fluorescence, Molar incisor hypomineralization, Remineralization.
INTRODUCTION
The term molar incisor hypomineralization (MIH) is used to describe the clinical appearance of enamel hypomineralization of systemic origin affecting one or more first permanent molars (FPMs) that are associated frequently with affected incisors.1 Recent literature has reported it as a relatively common condition with a pooled global prevalence of 14.2%.2,3 The prevalence of MIH in Chandigarh, India has been reported to be 11.72% in 8–12-year-old children and 6.3% among 6–9-year-old children.4 The condition is attributed to the disrupted ameloblastic function during the transitional and maturational stages of amelogenesis.5 The exact etiology remains unclear due to the lack of exact causal effect relationship of the various conditions and illnesses predisposing to the risk for MIH. It is a qualitative defect and the affected teeth have enamel that is soft, porous with white, yellow, or brown discoloration on the surface. These discolored areas represent areas of varying degrees of hypomineralization.6In vitro assessment of the microstructure and chemical composition of these defects have revealed more disorganized crystals with reduced relative mineral content.7 The dramatic reduction in the mechanical properties of FPM teeth has ramifications when clinicians are choosing restorative materials to restore the defects. The reason for the dramatic reduction in mechanical properties of hypomineralized FPM teeth is at present unknown and its treatment planning is usually guided by the type and severity of the defect. In “mildly” affected cases, where the enamel appears to be of good quality, fissure sealants, or the application of remineralizing agents are the treatment of choice. Composite restoration/onlays have been recommended in the literature as restorative treatment option in “moderate” cases, where the enamel/dentine defect is well demarcated and confined to one or two surfaces.2 However, in the “severe” form of MIH, where there is the involvement of two or more cusps, with or without pulpal involvement, the treatment options are very limited.
Since its establishment as an independent entity among the other developmental defects of enamel, the diagnosis of MIH has primarily been based on visually assessed criteria which bring with its subjectivity. Recently, however, the use of laser fluorescence (LF) in the form of Diagnodent has come up as a quantifiable measure of the hypomineralization in MIH-affected teeth. Higher LF scores are positively correlated with the increasing grades of MIH-associated surface opacities (highest for brown opacities and lowest for creamy white opacities). These findings implicate Diagnodent as a useful tool in the assessment of the mineralization status of tooth surfaces.
The treatment of the intact opacities in MIH-affected teeth is aimed at the prevention of their breakdown, as is commonly seen in such teeth. Various remineralization strategies originally employed for initial carious lesions have been extrapolated for use in developmentally hypomineralized teeth including the use of agents like fluoride varnish, CPP-ACP pastes, tri-calcium phosphate pastes, etc.
The present pilot study was thus planned with the aim to comparatively evaluate the remineralization of MIH-affected teeth by CPP-ACP-based cream and fluoride varnish, using LF.
MATERIALS AND METHODS
The two-parallel arm, open-label, prospective clinical trial was approved by the institutional ethics committee of the institute. The study was conducted on children attending the outpatient department of pedodontics and preventive dentistry of the institute.
A convenient sample of 30 children aged 8–14 years who exhibited intact, white, yellow, and brown color demarcated opacities of on their FPMs or permanent incisors that were consistent with the diagnostic criteria for MIH1 (Fig. 1), and the mean Diagnodent cut-off score >10 at baseline were included in the investigation, after taking informed consent from the concerned parents. All the patients received basic diet and oral hygiene instructions. Children with concomitant presence of any debilitating systemic disorder or on medication for a prolonged period were not included.
The selected teeth in these 30 children were then randomized via a simple randomization technique to receive one of the two remineralization interventions to prevent the selection bias and to eliminate the source of bias. The two study groups were:
Group I: after drying the teeth, 0.5 mL of varnish was applied with a single-tufted brush initially on the lower arch followed by the upper arch, and participants were discharged with clear instructions, not to eat or drink anything at all for 2 hours and not to eat anything solid but take liquids/semisolids till next morning for maintaining prolonged contact between varnish and tooth surface. Group II: a single daily application of 0.3 g (pea size) of CPP-ACP cream was done by the participants at night time to maintain a prolonged contact of this agent with the tooth surface. A standardized measuring scoop was given to each participant, to ensure the delivery of 0.3 g of CPP-ACP to the enamel slabs by each participant. Blinding was also not possible as these two agents differ in their mode of application and physical properties.
After performing oral prophylaxis, the mineral density of the affected teeth was determined using a DIAGNOdent™ pen (KaVo) at baseline such that the highest and the lowest fluorescence scores were recorded on the tooth exhibiting the most severe, intact hypomineralization defect in the entire dentition. Mineral density of 30 teeth with MIH, but without signs of post-eruptive breakdown was thus, assessed using DIAGNOdent (KaVo, Biberach, Germany) by a single operator who was calibrated in the use of the device and who calibrated the instrument before each reading as per the manufacturer’s recommendations. Laser fluorescence of these lesions was then recorded after 15 days, once again noting the maximum and the minimum fluorescence readings. The overall 15-day study duration was decided based on the literature on the use of CPP-ACP which have shown a statistically significant increase in mineral content and enamel surface microhardness as well.8
In the present study, comparison with an unaffected tooth in the same dentition was not possible because, after application, the remineralizing solution dissolves into the saliva and thus, interacts with the entire dentition. The detailed methodology has been summarized in Flowchart 1.
STATISTICAL ANALYSIS
Descriptive and inferential statistical analysis was done in the present study by using SPSS version 18 (IBM Corporation, SPSS Inc., Chicago, IL, USA). Results on the continuous measurement will be presented on mean ± SD. The normality of the data will be assessed using the Shapiro–Wilk test. The difference within a group over some time was assessed using the Wilcoxon signed-rank test and between the group using the Mann–Whitney U test. A p value of <0.05 will be considered to be significant, two-tailed.
RESULTS
At baseline, the normality was assessed using Kolmogorov–Smirnov and Shapiro–Wilk test and there was no significant difference and thus, it was assumed the samples were uniformly distributed among the two groups.
Table 1 shows the mean values, standard deviation, and ranges of LF readings for the two groups at baseline and 15 days post-application of the remineralizing agents. The distribution of defects in the two groups was largely uniform with no statistically significant difference observed between the two groups at baseline.
The mean value of LF recorded in group I was 29.27 ± 18.006 and that for group II was 26.87 ± 14.157 at baseline (Flowchart 1). After 15 days, post-application of the remineralizing agents the LF scores of both the groups showed a decrease (Fig. 2). The mean change was 8.933 ± 5.05 for the fluoride varnish group and 7.133 ± 4.17 for the CPP-ACP group (Fig. 3). This decrease was statistically significant for both groups. However, no significant difference was found between the two groups in terms of these changes. There was no change in color of these demarcated opacities after post-application of two remineralizing agents.
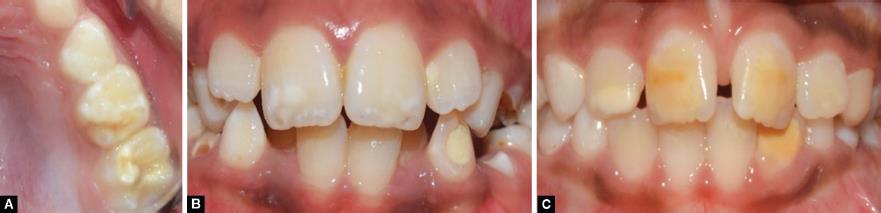
Figs 1A to C: Clinical intraoral photographs of hypomineralized enamel of MIH-affected molars and incisors

Flowchart 1: Detailed flow diagram of the methodology

Fig. 2: Comparison of mean fluorescence scores at baseline and after 15 days of post-application

Fig. 3: Comparison of mean change in fluorescence after application of two remineralizing agents
| Time interval | Group I (fluoride varnish) | Group II CPP-ACP | Z value | p value |
|---|---|---|---|---|
| Baseline | 29.27 ± 18.006 | 26.87 ± 14.157 | −0.104 | 0.917 |
| Day 15 | 20.33 ± 14.036 | 19.73 ± 4.174 | −0.166 | 0.868 |
| Difference | 8.933 ± 5.05 | 7.133 ± 4.17 | −0.958 | 0.338 |
| p value (baseline vs post 15 days) | 0.001 | 0.001 |
DISCUSSION
Based on the findings of the in vitro studies, the severity of the hypomineralized defect can be assessed using LF as an indicator of mineral density and is effective in the quantitative assessment of remineralization on smooth enamel surfaces. It allows non-invasive estimation of mineral density and the severity of the enamel defects at baseline before treatment and then evaluating the effectiveness of products commonly used to treat caries-related lesions.9
Molar incisor hypomineralization has been described as a qualitative defect resulting from a disruption of the ameloblasts during the early maturation stage of amelogenesis due to any one of several possible etiological factors.5 These areas of defective mineralization clinically manifest as opacities on the surfaces of affected molars and incisors, which may further undergo breakdown under masticatory forces.6 The assessment of these opacities is usually done visually and can have the problem of subjectivity. Recently the use of LF in determining the mineral density of MIH-affected teeth has been reported with considerable success. Fridman et al.10 have shown a lower mineral density as recorded by LF in clinically intact enamel of MIH patients than in patients without MIH. And the relation between visual changes of enamel color and LF readings was also observed.10
The treatment of MIH-affected teeth depends predominantly on the severity of the hypomineralization defect. While affected teeth that exhibit post-eruptive breakdown are subjected to restorative treatment options, the intact defects are approached with more conservative attempts at reinforcing and protecting the existing dental structure.3 Several remineralization strategies that were originally developed for white spot lesions have also been proposed for use in hypomineralized defects with mixed results. The efficacy of fluoride varnish in promoting the remineralization of artificially induced carious lesions has been shown by Bharti et al.11 who assessed the effect of fluoride varnish on artificially induced carious lesions under polarized microscopy. Savas et al.12 found a significant increase in calcium, phosphorous, and fluoride content in white spot lesions, 4 weeks after a single application of 2.26% fluoride varnish. According to Memarpour et al.,13 oral hygiene along with four fluoride varnish applications or constant CPP-ACP during the 12 months reduced the size of WSL in the anterior primary teeth and caused a small increase in dmft index values, whereas Llena et al.14 have reported CPP-ACFP is superior to fluoride varnish at remineralizing smooth-surface WSLs.
Limited literature was available on the use of remineralizing agents on hypomineralized lesions. However, some of the authors have applied and reported their findings like Restrepo et al.15 found no significant differences in QLF scores of MIH lesions after treatment with four applications of NaF varnish. However, Biondi et al.8 reported a significant decrease in DIAGNOdent scores of MIH-affected tooth surfaces after 15 days of NaF varnish application for 1 minute. The same study also reported a significant decrease in the scores after treatment with CPP-ACP paste. Similar results in favor of CPP-ACP paste have also been reported by Bakkal et al.16 Sezer et al.17 have shown a significant change in Diagnodent pen scores from baseline to 3 months after regular application of CPP-ACPF (GC MI Paste Plus) on hypomineralized enamel of MIH-affected anterior teeth. The increase in calcium and phosphorus content of hypomineralized enamel slabs of MIH-affected teeth could be due to its porous nature which acts as a permeable membrane to small ions like Ca2+, P+ thus leading to their accumulation.18
Though Biondi et al.,8 Ozgul et al.,19 Bakkal et al.,16 and Pasini et al.20 reported positive results after applying CPP-ACP pastes, its effectiveness as desensitizing and remineralizing agent has been questioned and long-term clinical trials with large samples are needed to validate the results before its widespread recommendation.
Only a limited amount of literature is available on the efficacy of these remineralizing agents on MIH-affected teeth. An increase in calcium and phosphorus content of MIH-affected teeth was seen after regular application of CPP-ACP cream over 3 years as observed by SEM and EDS analysis.21 However, fluoride varnish application on MIH-affected teeth every 1 week for 1 month did not show any significant changes in mean levels of fluorescence, possibly as in this study mineral content of teeth was not directly analyzed and only an indirect assessment of remineralization was done through measuring the change in the level of fluorescence.8 CPP-ACP, fluoride varnish, and ozone have been used by Ozgul et al.19 to decrease hypersensitivity of MIH-affected teeth and he found CPP-ACP with ozone to be the most effective in reducing the hypersensitivity followed by CPP-ACP alone and fluoride varnish.19
CONCLUSION
The following conclusions can be drawn from the present trial:
There was no significant difference between the two groups in terms of change in mean fluorescence scores, after 15 days of their applications. So, it could be assumed that both CPP-ACP cream and fluoride varnish are equally effective in achieving remineralization of MIH-affected teeth. CPP-ACP is also perceived as a safer measure due to the skepticism among parents surrounding the use of fluoride in children.
LIMITATIONS AND FUTURE PROSPECTS
Fluoride varnish has an advantage over CPP-ACP cream as it does not require any compliance on the part of the patients through CPP-ACP has an advantage of being a home care measure and hence does not require a visit to a dental clinic. But compare to material cost-effectiveness, CPP-ACP found to be costly. The major limitation of the present study is its sample size and short follow-up period. To reach a more conclusive finding similar study may be planned on a larger sample for a longer duration. Lack of standardization of the defects is another limitation of the study, as it could not be possible due to varying mineral content of these localized demarcated opacities. Future research focusing on in vivo studies on the effect of remineralizing agents on MIH-affected enamel might justify their use in improving the mineral content of the hypomineralized enamel.
REFERENCES
1. Weerheijm KL, Duggal M, Mejàre I, et al. Judgement criteria for molar-incisor hypomineralization (MIH) in epidemiologic studies; a summary of the European meeting on MIH held in Athens 2003. Eur J Paediatr Dent 2003;4(3):110–113.
2. Lygidakis NA. Treatment modalities in children with teeth affected by molar-incisor enamel hypomineralization (MIH): a systematic review. Eur Arch Paediatr Dent 2010;2(2):65–74. DOI: 10.1007/BF03262715.
3. William V, Messer LB, Burrow MF. Molar incisor hypomineralization: review and recommendations for clinical management. Pediatr Dent 2006;28(3):224–232.
4. Mittal NP, Goyal A, Gauba K, et al. Molar incisor hypomineralisation: prevalence and clinical presentation in school children of the northern region of India. Eur Arch Paediatr Dent 2014;15(1):11–18. DOI: 10.1007/s40368-013-0045-4.
5. FDI Commission on Oral Health Research and Epidemiology. A review of the development defects of enamel index: DDE Index. Int Dent J 1992;42:411–426.
6. Jalevik B. Prevalence and diagnosis of molar-incisor-hypomineralization (MIH). A systematic review. Eur Arch Paediatr Dent 2010;10(2):59–64. DOI: 10.1007/BF03262714.
7. Fearne J, Anderson P, Davis GR. 3D X-ray microscopic study of the extent of variations in enamel density in first permanent molars with idiopathic enamel hypomineralisation. Br Dent J 2004;196(10):634–638. DOI: 10.1038/sj.bdj.4811282.
8. Ana B, Silvina C, Lucia B, et al. Comparison of mineral density in molar incisor hypomineralization applying fluoride varnishes and casein phosphopeptide-amorphous calcium phosphate. Acta Odontolog Latinoamericana 2017;30:118–123.
9. Moriyama CM, Rodrigues JA, Lussi A, et al. Effectiveness of fluorescence based methods to detect in situ demineralization and remineralization on smooth surfaces. Caries Res 2014;48(6):507514. DOI: 10.1159/000363074.
10. Fridman D, Cortese SG, Biondi AM. Clinical Aspect and Reduction in Mineral Density using Laser Fluorescence in Hypomineralization. J Dent Res Abstract Archives. Argentine Division Meeting (Argentina): 95, 2013. URL: https://iadr.abstractarchives.com/abstract/argentine13193288/clinical aspect and reduction in mineral density using laser fluorescence in hypomineralization.
11. Bharti MNP, Aminah M, Singh P. Effect of laser and fluoride application for remineralization of the carious lesion: a polarized microscopic study. Int J Contemp Med Res 2017;4(2):489–492.
12. Savas S, Kavrìk F, Kucukyìlmaz E. Evaluation of the remineralization capacity of CPP-ACP containing fluoride varnish by different quantitative methods. J Appl Oral Sci 2016;24(3):198–203. DOI: 10.1590/1678-775720150583.
13. Memarpour M, Fakhraei E, Dadaein S, et al. Efficacy of fluoride varnish and casein phosphopeptide-amorphous calcium phosphate for remineralization of primary teeth: a randomized clinical trial. Med Princ Pract 2015;24(3):231–237. DOI: 10.1159/000379750.
14. Llena C, Leyda AM, Forner L. CPP-ACP and CPP-ACFP versus fluoride varnish in remineralisation of early caries lesions. A prospective study. Eur J Paediatr Dent 2015;16(3):181–186.
15. Restrepo M, Jeremias F, Santos-Pinto L, et al. Effect of fluoride varnish on enamel remineralization in anterior teeth with molar incisor hypomineralization. J Clin Pediatr Dent 2016;40(3):207–210. DOI: 10.17796/1053-4628-40.3.207.
16. Bakkal M, Abbasoglu Z, Kargul B. The effect of casein phosphopeptide-amorphous calcium phosphate on molar-incisor hypomineralisation: a pilot study. Oral Health Prev Dent 2017;15(2):163–167. DOI: 10.3290/j.ohpd.a37928.
17. Sezer B, Caliskan C, Durmus B, Efficacy of MI Paste for Remineralization in MIH-Affected Incisors: A 3-months Clinical Study.(Abstarct).
18. Bertacci A, Chersoni S, Davidson CL, et al. In vivo enamel fluid movement. Eur J Oral Sci 2007;115(3):169–173. DOI: 10.1111/j.1600-0722.2007.00445.x.
19. Ozgul BM, Saat S, Sonmez H, et al. Clinical evaluation of desensitizing treatment for incisor teeth affected by molar-incisor hypomineralization. J Clin Pediatr Dent 2013;38(2):101–105. DOI: 10.17796/jcpd.38.2.92mx26l6n482j682.
20. Pasini M, Giuca MR, Scatena M, et al. Molar incisor hypomineralization treatment with casein phosphopeptide and amorphous calcium phosphate in children. Minerva Stomatol 2018;67(1):20–25. DOI: 10.23736/S0026-4970.17.04086-9.
21. Baroni C, Marchionni S. MIH supplementation strategies: prospective clinical and laboratory trial. J Dent Res 2011;90(3):371–376. DOI: 10.1177/0022034510388036.
________________________
© The Author(s). 2021 Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (https://creativecommons.org/licenses/by-nc/4.0/), which permits unrestricted use, distribution, and non-commercial reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The Creative Commons Public Domain Dedication waiver (http://creativecommons.org/publicdomain/zero/1.0/) applies to the data made available in this article, unless otherwise stated.